
“Unlike a colonoscopy, one typically does not have to consume an oral lavage solution to entirely clean out the colon,” Click explains. 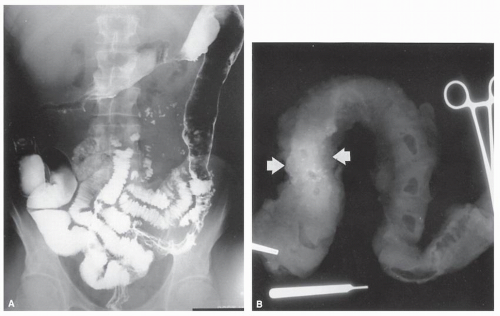
But it’s only extended through the left side of your colon, which consists of the two areas leading up to your rectum: the descending colon and the sigmoid colon.īecause it only involves the last few segments of your colon, a sigmoidoscopy doesn’t require as much preparation as a colonoscopy. Click says, a scope is inserted through your anus to examine your anal canal, rectum, and colon. “The way I describe it to patients is a ‘half-colonoscopy,’” explains Benjamin Click, MD, a gastroenterologist at the UCHealth Digestive Center in Aurora, Colorado. The main difference between a sigmoidoscopy and a colonoscopy is how far the scope is inserted into your colon during the procedure. 1Įlevation in serial measurements of fecal calprotectin predicts relapse, whereas serial values in the normal range predict continued remission over time.Sigmoidoscopy vs. 1Įndoscopic evidence of continuous colonic inflammation starting at the rectum with confirmatory biopsies establishes the diagnosis of ulcerative colitis. Other tests, such as complete blood count, erythrocyte sedimentation rate, and measurement of C-reactive protein, may be useful but are nonspecific. difficile toxin assay and stool examination for ova and parasites, should be performed. 9, 11īacterial stool culture, including C. Therefore, in children with a negative fecal calprotectin test, endoscopy can be limited to those whose symptoms persist without another diagnosis. 10 A normal fecal calprotectin level (100 mcg per g or less) in children virtually excludes the diagnosis of ulcerative colitis (100% negative predictive value 95% CI, 98% to 100%). 1, 9įecal calprotectin testing has a high negative predictive value and helps to differentiate inflammatory bowel disease from irritable bowel syndrome, but no serum biomarkers alone are sufficient for the diagnosis of ulcerative colitis. Lower endoscopy should be performed on all adult patients with suspected ulcerative colitis. Monitor patients with ulcerative colitis for dysplasia and malignancy with follow-up colonoscopy every one to three years based on risk factors and prior endoscopy findings. 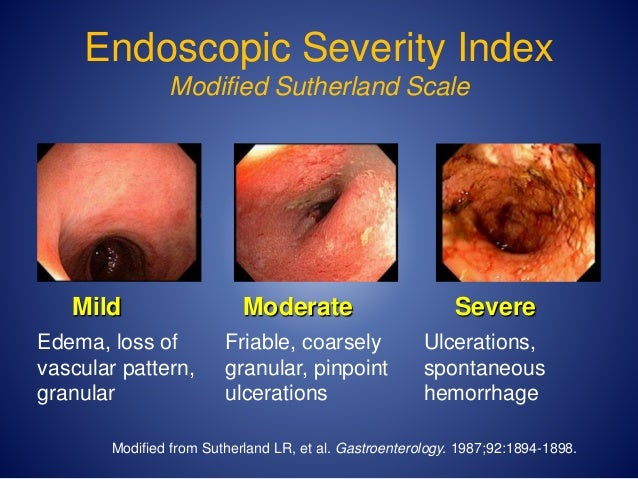
1, 13Īdd rectal mesalamine to oral 5-ASA therapy for patients with extensive mild to moderate ulcerative colitis. Mesalamine is more potent than sulfasalazine. Use 5-ASA medications as initial therapy for mild to moderate ulcerative colitis. 10 However, a negative fecal calprotectin test largely rules out ulcerative colitis in children. 1, 9ĭo not use biomarker testing to diagnose ulcerative colitis. Children with a negative fecal calprotectin test are unlikely to have ulcerative colitis endoscopy can be limited to those whose symptoms persist without another diagnosis. Order lower endoscopy on all adult patients with suspected ulcerative colitis. Increased risk of colorectal cancer and use of immunosuppressive therapies affect the preventive care needs for these patients.Įxclude infectious colitis with stool culture and Clostridioides difficile toxin testing before diagnosing ulcerative colitis. Surgical treatment may be needed for fulminant or refractory disease. Other treatments such as fecal microbiota transplantation are considered experimental, and complementary therapies such as probiotics and curcumin have mixed data. Choice of medication and method of delivery depend on the location and severity of mucosal inflammation. Medications available to treat the inflammation include 5-aminosalicylic acid, corticosteroids, tumor necrosis factor–alpha antibodies, anti-integrin antibodies, anti-interleukin-12 and -23 antibodies, and Janus kinase inhibitors. Fecal calprotectin may be used to assess disease activity and relapse. Diagnosis is suspected based on symptoms of urgency, tenesmus, and hematochezia and is confirmed with endoscopic findings of continuous inflammation from the rectum to more proximal colon, depending on the extent of disease. 
Risk factors include recent Salmonella or Campylobacter infection and a family history of ulcerative colitis. Ulcerative colitis is a relapsing and remitting inflammatory bowel disease of the large intestine.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
